Forgetting dreams when waking up seemed like an unimportant anecdote. A Spanish macro-study has linked it to Alzheimer’s
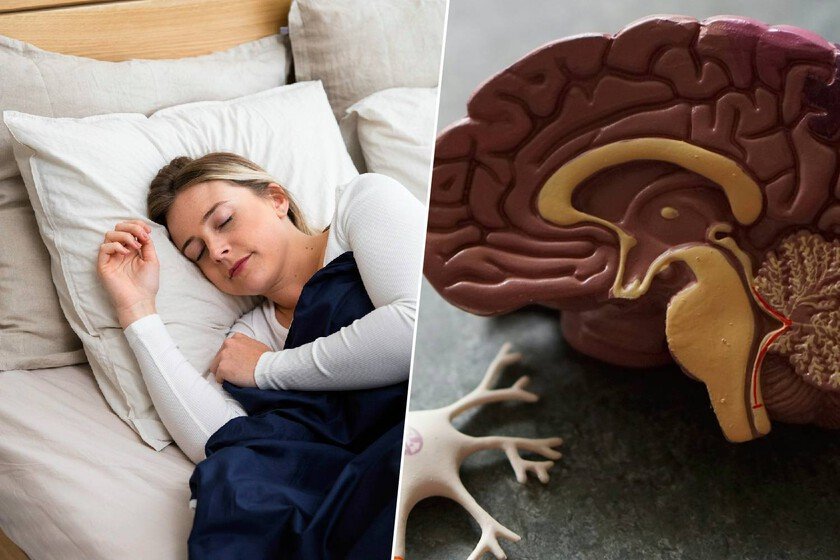
Today, one of the great challenges that modern neurology has with the Alzheimer’s It is not just treating it, but detecting it before it shows its face, since right now there are several therapeutic options that manage to stop the progression of the disease. That is why our effort is to find biomarkers that warn patients that something is happening, and the last one is related to dreams. Spanish research. Based on the Vallecas project and promoted by the Reina Sofía Foundation or the CEIN Foundationand who has pointed out how not remembering dreams can be a risk marker for Alzheimer’s very premature. But to reach this conclusion, researchers have had to analyze a cohort of 1,049 people cognitively healthy older adults, who have been closely followed for a period of up to 10 years. In the end we are talking about a large amount of information that has intersected with the genetics and lifestyle of all patients, and even with the moment in which the first molecular markers of Alzheimer’s began to appear. The dreams. At first glance it might seem like an anecdotal correlation that what happens with our dreams has some relationship with Alzheimer’s, but the reality is that it has a very solid neurobiological basis. And to understand it we have to go to what is known as the default neural network, which is a set of brain regions that are activated when our mind is at rest, wandering or precisely dreaming. Scientific evidence accumulated in recent years has shown that the default neural network is highly vulnerable to Alzheimer’s pathology and is, in fact, one of the first areas to suffer structural and functional damage. In this way, if this network begins to fail in the earliest phases of the disease, it is logical to think that functions associated with it, such as the consolidation and memory of dreams, will be diminished. They have gone further. One of the most interesting points of this Spanish study is that it was not based solely on patient surveys, which may have reduced reliability. Here the researchers looked for important biomarkers, such as the presence of the APOE ε4 allele, which is a genetic variant that predisposes one to suffer from the sporadic form of the disease. In addition, they also analyzed the tau-217 protein, which today is one of the blood markers that indicates a possible Alzheimer’s disease in the early stages of the disease. And only with a blood sample. That is why these results now gain greater strength when it comes to relating the problem to dreams and Alzheimer’s. A paradigm shift. Don’t be scared if you woke up this morning without remembering what you dreamed, since this is completely normal and depends on many factors such as stress, the sleep phase in which we wake up or even age. Here the researchers only point to a sustained pattern of loss of dream memory in older people who, so far, do not have any obvious cognitive problems. That is why this discovery is purely clinical and preventive, since scanning the entire population is unfeasible due to cost and risks. However, asking a patient in consultation about their sleeping habits and their ability to remember what they dream about is free and non-invasive. But logically this has to be accompanied by an effective screening system to be able to diagnose the disease even before the first serious symptoms appear. Images | Slaapwijsheid.nl Robina Weermeijer In Xataka | Dementia is devastating largely because it arrives without warning: some researchers already predict it seven years in the future